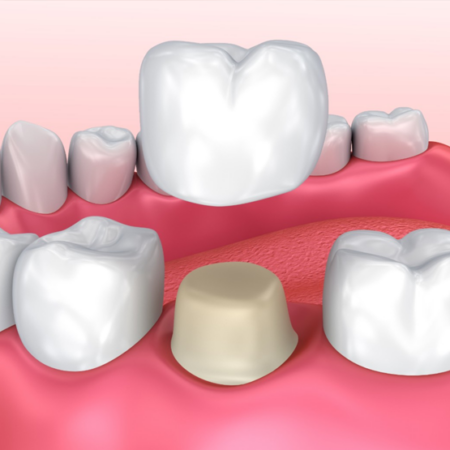
Endodontist vs. Periodontist: What’s the Difference?
You may be wondering what the difference is between an endodontist and a periodontist. Both are specialists in dentistry, but they have different areas of expertise. This blog post is dedicated to helping you become more informed on the difference between an endodontist and a periodontist.
An endodontist specializes in issues with the inside of teeth, while a periodontist specializes in issues with the gums and supporting bone structure. When should you see an endodontist vs. a periodontist? Keep reading to find out!
What is an Endodontist?
An endodontist is a dentist who specializes in diagnosing and treating issues with the pulp or nerve of the teeth and is especially helpful when you’re having tooth pain. An endodontist is an expert in endodontics (obviously), and endodontists go through additional training after dental school to become endodontists.
The most common procedure that endodontists perform is a root canal (we also refer to it as root canal therapy). During a root canal, endodontists remove the damaged or infected pulp from inside the tooth. They then clean and disinfect the inside of the tooth to help save the tooth (and make sure the pain goes away!).
Endodontists also treat cracked teeth, which can be caused by biting down on hard objects or trauma to the face. If you have a crack in your tooth, endodontists can place a filling or a crown to help restore your tooth and prevent further damage.
What is a Periodontist?
A periodontist is a dentist who specializes in diagnosing, treating, and preventing gum disease. They are experts in the field of periodontics.
Plaque, a sticky film of bacteria that forms on your teeth, causes gum disease. If you don’t remove plaque, it can harden into tartar and lead to inflammation of your gums. This early stage of gum disease is called gingivitis.
If gingivitis isn’t treated, it can progress into periodontitis. Periodontitis is a more serious form of gum disease that can damage the bones and tissues that support your teeth. Periodontitis can eventually lead to tooth loss, so it’s important to see a periodontist if you think you might have gum disease.
When should you see an endodontist vs. a periodontist?

If you’re experiencing any pain in your teeth or gums, it’s always a good idea to see your dentist first. They’ll be able to take a look and determine whether you need to see an endodontist or a periodontist.
Endodontists usually treat tooth pain that’s caused by infection, while periodontists usually treat gum disease. However, there is some overlap in their areas of expertise, so it’s always best to consult with your dentist first.
Are endodontists and periodontists also dentists?
Yep! Endodontists and periodontists are both types of dentists but with differences in what they specialize in regarding your teeth and mouth. Endodontists specialize in issues with the inside of teeth, while periodontists specialize in issues with the gums and supporting bone structure.
Your dentist possesses the training to diagnose such problems and can guide you to an endodontist or a periodontist, depending on the required treatment plan for your teeth.
How much extra training do endodontists and periodontists go through?
Both endodontists and periodontists go through extra training after they finish dental school. Endodontists complete a two- to three-year residency program in endodontics, while periodontists complete a three-year residency program in periodontics.
In their training, endodontists spend many hours learning how to diagnose and treat problems with the pulp of the tooth, such as infection or inflammation. They also learn how to perform root canals, which are procedures that remove the damaged pulp from the tooth.
What’s it like when endodontics meets periodontics?
Unfortunately, if a root canal infection goes untreated it can actually cause an abscess, or a pus swelling, in the jaw bone. This causes gum tenderness around your tooth, and a root canal may be necessary to treat the dental infection.
While this might not always require periodontal treatment, it does highlight how one issue can cascade into another. By removing the damaged or infected tissue inside the tooth, root canals can help restore the health of the gum tissue and prevent further damage to the tooth.