What Is Tooth Pulp?
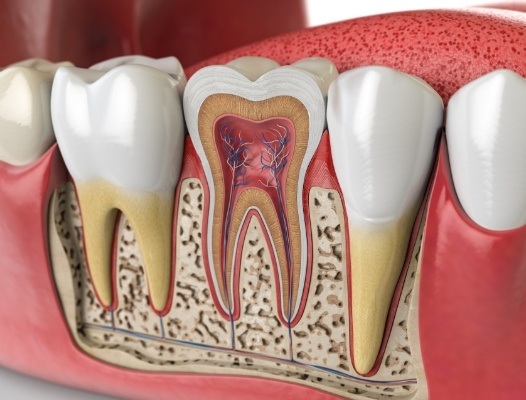
The pulp is the middle part of a tooth that contains nerves, blood vessels, and connective tissues. It is sealed off from the rest of a tooth in the innermost layer of the crown, called the pulp chamber. Any damage or decay that reaches this part of a tooth leaves soft tissues exposed to irritants in the mouth, like bacteria.
The dental pulp serves as your mouth’s natural alarm system when something is wrong with a tooth. For example, if it has been damaged, you will get a toothache. The pulp also plays a crucial role in the building of dentin. This is the second layer underneath a tooth’s enamel, and it contains tiny nerve endings.
The soft tissues that make up a tooth’s pulp play an essential role in its development, but teeth can survive without their pulp once fully grown. A matured tooth can extract nutrients from the tissues around it.
Root canal treatment for compromised tooth pulp
Root canal therapy is typically the first line of defense once a tooth’s pulp has been compromised. Tooth decay can penetrate into the pulp chamber, giving oral bacteria access to the nerves and connective tissues there. Injuries like a break or fracture can also leave a tooth’s pulp chamber exposed.
Issues with tooth pulp can lead to severe toothaches. The pain is often intense. Leaving a tooth with damaged pulp should never be an option because the tooth will eventually become infected by oral bacteria.
Root canal therapy
Root canal therapy enables dentists to save teeth with compromised pulp chambers. It has a reputation as a painful treatment, but that is inaccurate. Patients typically do not feel significant pain during the treatment because local anesthetics are used. In fact, any toothache that the patient was dealing with should be gone by the time that the procedure is over.
The treatment starts with the dentist injecting a local anesthetic into the area around the damaged tooth. A dental drill is used to make a hole into the pulp, and files are used to remove the soft tissues inside it. Medication is placed into the cavity before sealing it up with a material called gutta-percha.
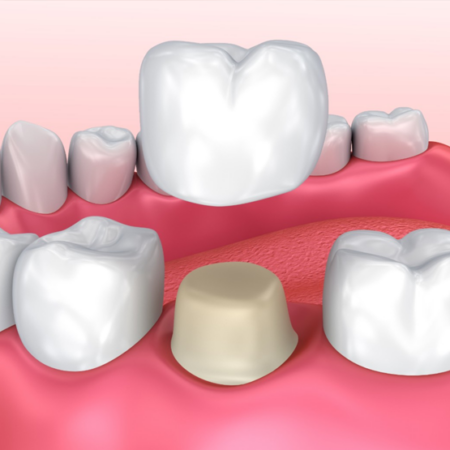
The restored tooth is usually covered with a crown to protect it and restore its appearance. The entire process typically takes less than an hour.
Extraction
If a tooth with a compromised pulp is already severely infected, the dentist might recommend extracting it. This is a last-resort treatment, used only when the dentist thinks that a root canal would not effectively stop the spread of the infection.
Frequently asked questions about root canal therapy
Many patients are unsure if they need a root canal. Let us take a look at a few frequently asked questions about this procedure.
1. Do root canal treatments hurt?
No. While popular conception suggests otherwise, that is not the case for most patients. Root canal therapy was indeed quite the ordeal before the invention of anesthesia. But nowadays, patients do not feel much during their treatments because local anesthetics are administered at the start of the procedure. These numb the regions in the mouth being worked on, preventing the patient from feeling pain.
To put it succinctly, root canal treatments do not cause pain. Instead, they end the pain caused by a compromised pulp chamber.
2. Is root canal therapy always the ideal solution?
No, it depends on the severity of the damage or infection affecting the tooth. For example, an extraction might be recommended if there is a significant risk of infection spreading to other parts of the body. An infected tooth may not be a huge deal at first, but it can become one if the infection reaches more sensitive parts of the body, like the brain and heart.
3. What are common signs that I need a root canal?
Root canal therapy is typically suggested when a tooth has a compromised pulp chamber. The pulp contains soft tissues like nerves, connective tissues, and blood vessels. Decay or trauma opening up this area often leads to extreme toothaches that are impossible to ignore.
Other symptoms of a damaged pulp chamber include increased teeth sensitivity, bad breath, pus coming from around a tooth, a tooth darkening, and swollen gum tissues at the base of the affected tooth.







Pingback: Soft Teeth: The Facts You Need to Know -